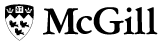Making new heart muscles
A year and a half ago, Ray Chiu was up to his neck in research on skeletal muscle cells. But an article about a breakthrough in Japan made him abruptly change course.
 Professor Ray Chiu
Professor Ray ChiuPHOTO: Owen Egan |
|
"A Japanese scientist showed that bone marrow stromal cells -- also known as stem cells -- can turn into heart muscle in the Petri dish. The moment I read that, as a surgeon I saw the clinical applications. We immediately shifted all of our efforts into bone marrow research."
Professor Chiu, chair of the Division of Cardiothoracic Surgery at the McGill University Health Centre, hasn't wasted any time since.
In a widely reported presentation at an American Heart Association conference in New Orleans earlier this week, Chiu described successful stem cell experiments in lab rats. Working with graduate students and McGill molecular biologist Jacques Galipau, Chiu has developed a technique in which he extracted bone marrow cells from rats with heart failure, and then injected them directly into the animals' hearts. The result was viable new heart muscle.
Chiu feels that the time is right to look at stem cells as a versatile source of therapy.
"Stem cells have the ability to differentiate, or turn into, virtually any type of cell in the body -- brain cells, kidney cells, liver, etc. They are guided by the microenvironment where they find themselves. Thanks to this ability, stem cells can be of interest to anyone treating conditions causing damage to existing cells, particularly those that cannot reproduce or repair themselves."
Recent discoveries have challenged the traditional scientific view that bone marrow has only one function: to produce white and red blood cells. Marrow stromal cells were thought to support this process.
"But in recent years we have come to recognize that stromal cells are actually adult stem cells, as opposed to embryonic stem cells .... My evolutionary theory is that they developed as a reserve for body repair."
Chiu believes that many other researchers in diverse fields will take up the gauntlet now that he has shown the potential of stem cells. But few areas hold as much potential to change lives as heart research because of the heavy annual toll from heart conditions.
"Incidences of heart disease have been declining in our society for the last 20 years, because we are better at risk management; we eat better, exercise more. But heart failure rates have been increasing. In fact, it is the most common diagnosis made on adult patients in North America. Heart failure can be caused by heart attacks, viral infections or other problems, but the common denominator is that heart muscles die.
"Unfortunately, the heart muscles lose the ability to divide and repair themselves after we are born -- they can only become bigger."
Chiu notes that heart failure is not always fatal, thanks to better drugs and treatment, but patients tend to live their lives in and out of hospitals and intensive care units. Chiu's research holds out the possibility -- if the procedure proves safe and effective in humans -- of restoring healthy heart muscle.
In addition, the therapy would be an alternative to using embryos.
"When most people hear about stem cells, they think about embryonic stem cells. There is still opposition against this type of research. But if I can use my patients' own stem cells, I avoid using embryos."
In fact, the benefits would be multiple, which Chiu has no trouble listing one by one.
"I'm not doing a heart transplant, so I don't need to wait for a donor. Because I'm using the patient's own cells, there is no risk of rejection, so I don't have to use immuno-suppressive drugs. This is a renewable resource; the body quickly replaces any which are removed from the bone marrow. And the procedure is not invasive; it can be done with a needle to extract the cells, and a needle or catheters in the arteries to introduce it in the heart."
Chiu expects that the Food and Drug Administration in the US and Health Canada will approve human trials early next year.
"I believe it will take at least two years for this procedure to come into clinical practice. But if patients exert pressure to speed up the process, that could speed things up. I know that lots of patients with nothing to lose will volunteer for the trials."
Chiu will report his findings in the November or December issue of the journal Thoracic and Cardiovascular Surgery.